History of Present Illness
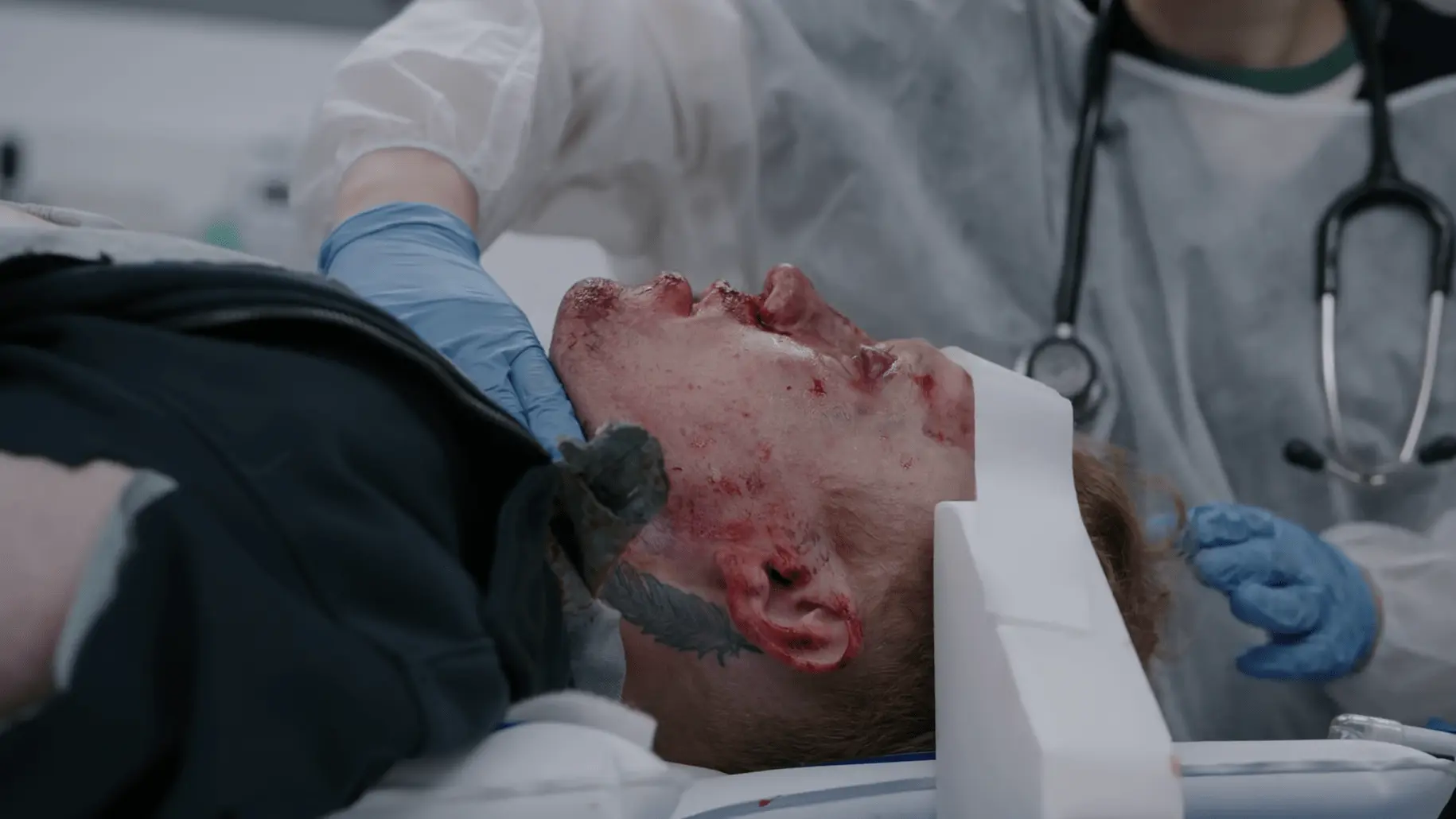
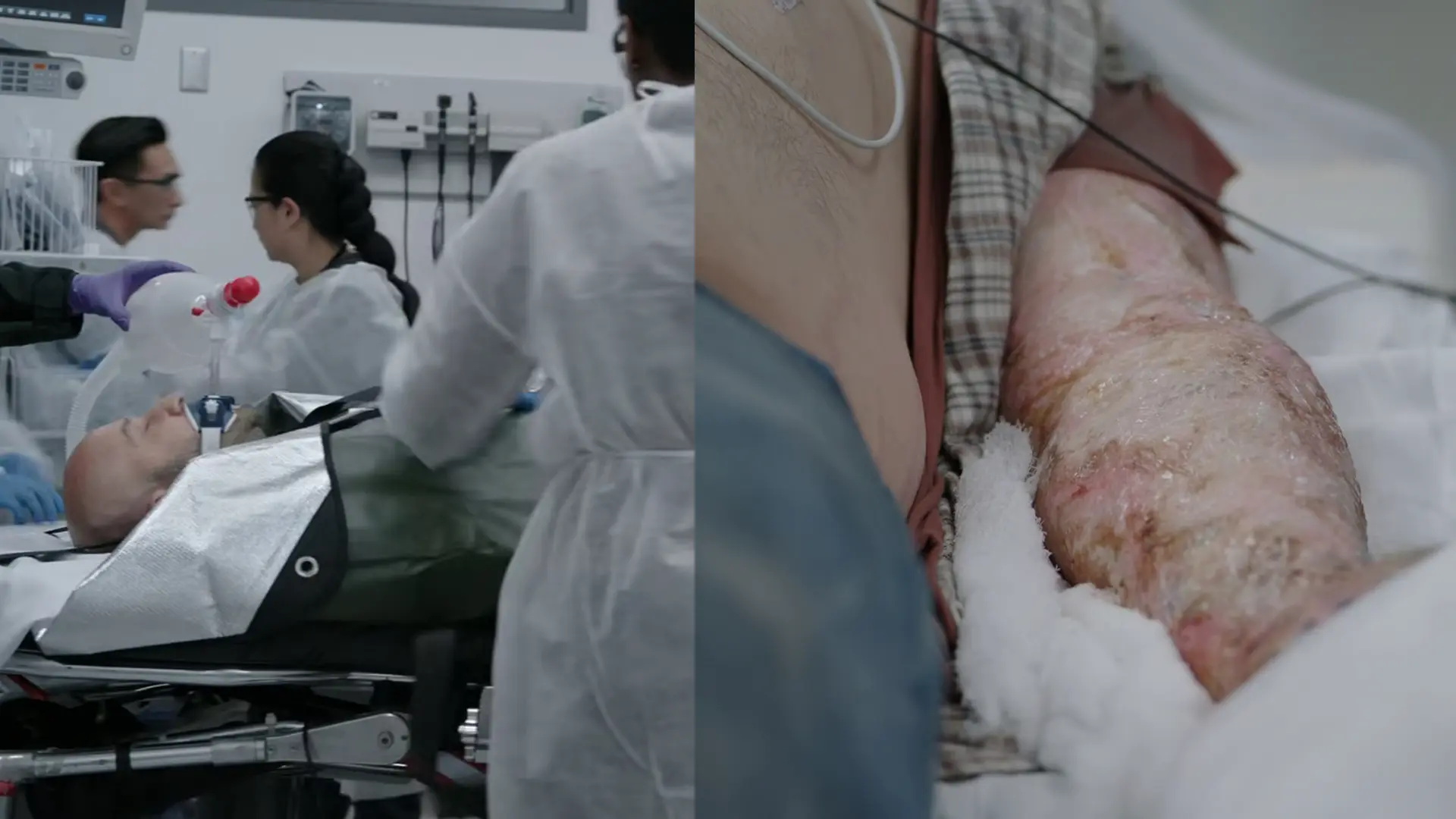
19-year-old college student found unresponsive in his bed by his mother. No known medical history, no daily medications, no known allergies. Found barely breathing with pinpoint pupils and a heart rate of 38. Prehospital EMS administered Narcan which improved pupillary response, but the patient failed to breathe spontaneously and required endotracheal intubation. No obvious signs of trauma, and no drugs or alcohol were reported on the scene.

Emergency Department Course
Initial Evaluation & Resuscitation
Patient arrival via EMS, unresponsive and intubated.
+1
Initial Evaluation & Resuscitation
Patient arrival via EMS, unresponsive and intubated.
Medical Decision Making
Considering toxidromes vs. primary neurologic event vs. trauma. Opiate overdose fits the initial pinpoint pupils, but failure to regain respiratory drive post-Narcan suggests prolonged hypoxia leading to brain injury. Beta blockers wouldn't explain the pinpoint pupils. Need to evaluate brainstem reflexes to determine the extent of neurologic damage.
Diagnostics & Findings
- Pupillary exam
- Pain stimulus response check
Findings:
- Pupils 6mm and non-reactive
- No response to pain
- GCS 3
Interventions
- Mechanical ventilation (continued from EMS)
⮑ Outcome & Reassessment
Patient remains deeply comatose, flaccid, and unresponsive.
Clinical Media

Neurological Reassessment
Continuing primary survey to establish a neurologic baseline before CT scan.
+1
Neurological Reassessment
Continuing primary survey to establish a neurologic baseline before CT scan.
Medical Decision Making
With a GCS of 3 and fixed/dilated pupils, I need to check for remaining brainstem function. The oculovestibular reflex (cold caloric test) tests the integrity of the brainstem. The absence of response confirms severe hypoxic injury or massive intracranial hemorrhage.
Diagnostics & Findings
- Ice water caloric test (oculovestibular reflex)
Findings:
- Flaccid paralysis of all four extremities
- No eye movement with ice water
Interventions
- Preparation for transport to CT scanner
⮑ Outcome & Reassessment
Patient demonstrates total absence of brainstem reflexes. Sent to CT with a drug box and continuous monitoring.
Clinical Media
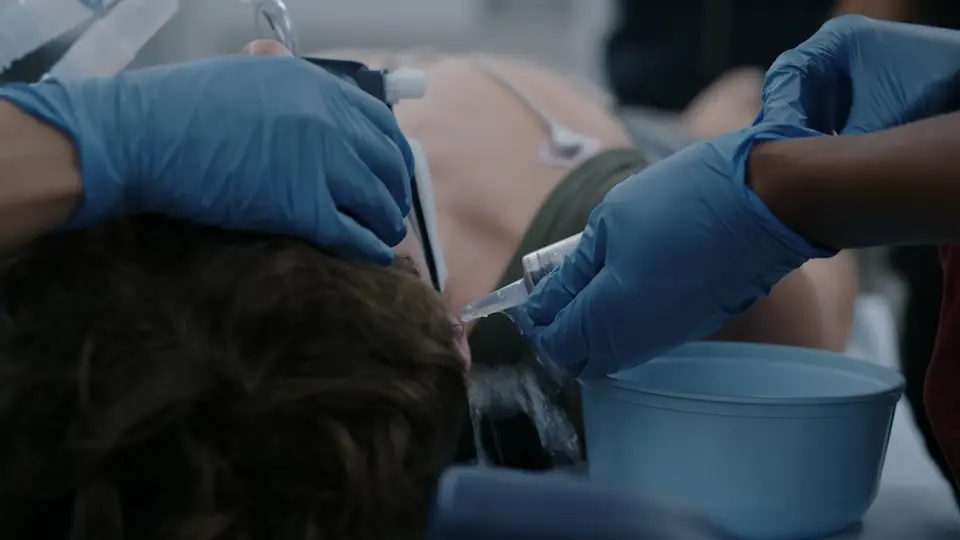
Lab Review & Family Education
Return of Head CT results and Urine Drug Screen (UDS). Parents present at bedside.
Lab Review & Family Education
Return of Head CT results and Urine Drug Screen (UDS). Parents present at bedside.
Medical Decision Making
Head CT is normal, which rules out massive hemorrhage and confirms anoxic brain injury as the cause of brainstem failure. UDS is positive for fentanyl, explaining the initial respiratory arrest. Need to educate the family that fentanyl is frequently found in counterfeit prescription pills (like Xanax or Ativan), which explains why an otherwise 'good kid' suffered an opioid overdose.
Diagnostics & Findings
- Head CT
- Urine Drug Screen (UDS)
Findings:
- Head CT: Normal (no acute intracranial hemorrhage)
- UDS: Positive for Fentanyl
Interventions
- Family counseling and emotional support
⮑ Outcome & Reassessment
Patient condition unchanged. Parents initially in denial regarding drug use, but accept the information and are allowed to sit at the bedside.
End of Life / Brain Death Declaration Prep
Patient has had sufficient time for toxins to clear (with Narcan) but shows no neurologic recovery. Need to formalize the poor prognosis.
End of Life / Brain Death Declaration Prep
Patient has had sufficient time for toxins to clear (with Narcan) but shows no neurologic recovery. Need to formalize the poor prognosis.
Medical Decision Making
The clinical picture of absent cranial nerve activity and blown pupils following an anoxic event is practically diagnostic of brain death. However, strict legal and medical protocols require formal confirmatory testing to declare death: an apnea test and a cerebral perfusion study. Must prepare the family for the reality that their son will not wake up.
Diagnostics & Findings
- Ongoing serial neurologic exams
Findings:
- No cranial nerve activity
Interventions
- Discussed need for apnea test and cerebral perfusion study
- Delivered grave news to the parents
⮑ Outcome & Reassessment
Patient remains clinically brain-dead. The mother demonstrates severe grief and bargaining, pleading for the doctor to 'shock him back' and wake him up.
Diagnoses & Disposition
Evolving Diagnoses
- [S01E02]Opiate Overdose (Fentanyl)
- [S01E02]Severe Hypoxic-Ischemic Encephalopathy (Anoxic Brain Injury)
- [S01E02]Clinical Brain Death
Current Disposition
Admitted to ICU for formal brain death criteria testing (apnea test, cerebral perfusion study) and likely evaluation for organ donation.
Casebook Analysis
Episode Context
Nick's case operates as the tragic emotional anchor of the episode, highlighting the pervasive and unpredictable nature of the modern fentanyl epidemic where college students inadvertently overdose on counterfeit pills. It serves to emphasize the emotional toll emergency medicine takes on providers and families.
Attending's Review
Medical Accuracy
The medical depiction is highly accurate and clinically sound. Pre-hospital pinpoint pupils that become blown and fixed 6mm pupils on arrival perfectly illustrate a patient whose opiate toxicity triggered respiratory arrest, which subsequently caused irreversible anoxic brain injury. The mention of cold water calorics to test the brainstem, and the specific requirements for declaring brain death (apnea test, cerebral perfusion study), are spot-on standard of care.
Complications & Errors
- There were no medical errors made by the ED team. The tragic outcome was entirely secondary to the prolonged anoxic downtime before the patient was discovered by his parents.
Clinical Pearls
Naloxone (Narcan) reverses the opioid toxidrome at the receptor level, but it cannot reverse anoxic brain injury sustained during prolonged respiratory depression.
The oculovestibular reflex (ice water caloric test) is a crucial, easily performed bedside test to evaluate lower brainstem function in comatose patients.
Counterfeit pills pressed with illicit fentanyl are a massive driver of unexpected overdoses, meaning a lack of known substance abuse history should never rule out a toxidrome.