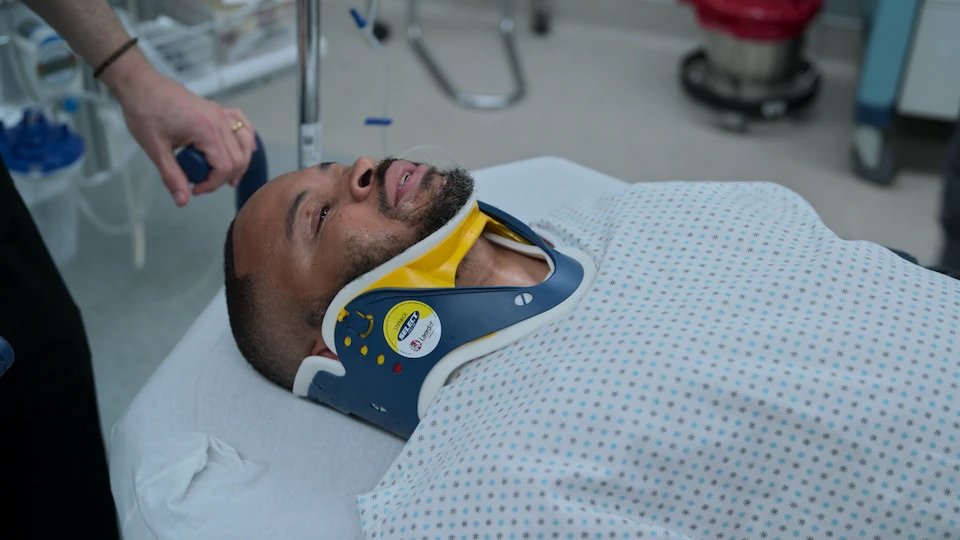
History of Present Illness
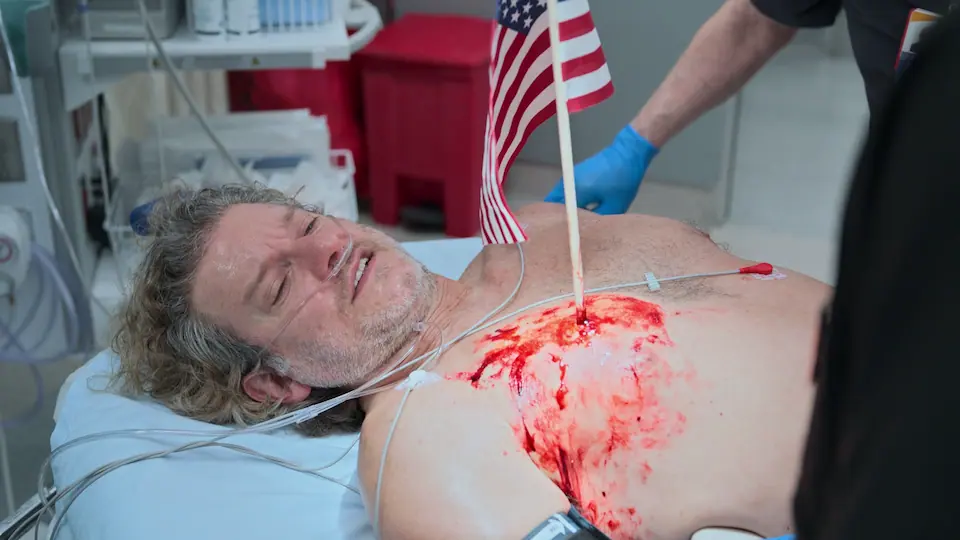
34-year-old male presents to the ED via EMS following a bar fight over a game of pool at a sports bar. He sustained a penetrating thoracic injury when an adversary impaled him in the right chest with an American flag pole. The object remains in situ. Patient is awake, alert, and combative on arrival.
Emergency Department Course
Triage & Initial Evaluation
EMS arrival with penetrating chest trauma.
Triage & Initial Evaluation
EMS arrival with penetrating chest trauma.
Medical Decision Making
Patient has a trans-thoracic impalement. The primary concern is tension pneumothorax, massive hemothorax, or direct cardiac/great vessel injury. The fact that he is hemodynamically stable (BP 132/87) with only mild tachycardia (112) is reassuring. The impaled object must be left strictly in place to prevent acute exsanguination from release of tamponade.
Diagnostics & Findings
Findings:
- American flag pole impaled in right chest
- Mild hypoxia resolving on high-flow oxygen
- Tachycardic but hemodynamically stable
Interventions
- Placed on 15L O2 via Non-Rebreather mask
- Stabilization of impaled object
⮑ Outcome & Reassessment
Patient is highly agitated, yelling at his adversary across the trauma bay.
POCUS Assessment & Intervention Planning
Secondary survey and evaluation of pleural space integrity.
+2
POCUS Assessment & Intervention Planning
Secondary survey and evaluation of pleural space integrity.
Medical Decision Making
With an object impaled in the right hemithorax, a pneumothorax is highly likely. Bedside ultrasound (eFAST) confirms absent lung sliding, diagnosing a pneumothorax. The patient requires a chest tube to evacuate the pleural space and monitor for ongoing internal bleeding (hemothorax) prior to definitive operative extraction. A 20 French chest tube is selected.
Diagnostics & Findings
- POCUS (Point-of-Care Ultrasound) / eFAST
Findings:
- Absent lung sliding on the right, confirming right-sided pneumothorax
Interventions
- Prep for 20 French thoracostomy tube insertion
- Consultation for immediate OR transfer
⮑ Outcome & Reassessment
Patient expresses disbelief that he requires surgery, demanding the doctor just 'pull it out'. Doctor correctly refuses and preps him for the OR.
Clinical Media


Diagnoses & Disposition
Evolving Diagnoses
- [Triage & Initial Evaluation]Penetrating thoracic trauma
- [POCUS Assessment & Intervention Planning]Right-sided traumatic pneumothorax
Current Disposition
Transferred to Operating Room for extraction of foreign body and surgical exploration.
Casebook Analysis
Episode Context
Barrett Dunkle serves as the quintessential bizarre, highly visual holiday trauma designed to showcase the chaos of a 4th of July shift. His injury, humorously referred to as getting 'Iwo Jima'd', sets the tone for the frenetic pace the doctors are dealing with while being short-staffed.
Attending's Review
Medical Accuracy
The handling of the impaled object is highly accurate: the trauma team explicitly refuses the patient's demand to just 'pull it out', which is a critical real-world trauma tenet. Using POCUS to diagnose absent lung sliding is standard-of-care and extremely accurate. However, selecting a 20 French chest tube is slightly controversial; while recent literature supports smaller pigtail catheters (14F-20F) for pneumothoraces and even some hemothoraces, traditional ATLS guidelines often recommend larger tubes (28F-32F) if significant bleeding (hemothorax) is suspected to prevent the tube from clotting off.
Complications & Errors
- The ED environment is chaotic, with two combative patients placed near each other. In a real trauma center, security would isolate the combatants to prevent further escalation and maintain a safe clinical workspace.
Clinical Pearls
Never remove an impaled object in the Emergency Department. Objects act as a plug; removing them can release tamponade and lead to uncontrollable hemorrhage. Always stabilize the object and transfer to the OR.
The eFAST exam is highly sensitive for detecting pneumothorax. Absent lung sliding on B-mode, or the 'barcode/stratosphere sign' on M-mode, indicates the visceral and parietal pleura have separated.
Hemodynamically stable penetrating chest trauma without immediate indications for an ED thoracotomy (e.g., loss of vital signs with a narrow window) should be managed with tube thoracostomy and expedited transfer to the OR for definitive surgical exploration.
Optimal POCUS placement for pneumothorax evaluation: In a supine patient, free air will accumulate anteriorly. Place a high-frequency linear probe longitudinally (sagittal plane) in the mid-clavicular line, typically between the 2nd and 4th intercostal spaces. Visualize two adjacent ribs with their posterior acoustic shadowing to correctly identify the pleural line strung between them (the 'bat sign').