History of Present Illness
Patient awoke at 2:00 AM with intense upper abdominal pain that lasted approximately one hour and subsequently resolved. He reports eating a heavy, fatty meal (steak at Sullivan's) for his wife's birthday the night prior. He denies fever or vomiting. He has a history of hypertension but forgot to take his morning enalapril.

Emergency Department Course
Initial Evaluation & POCUS
Initial bedside triage and medical student assessment of a patient with resolved abdominal pain.
+1
Initial Evaluation & POCUS
Initial bedside triage and medical student assessment of a patient with resolved abdominal pain.
Medical Decision Making
The medical student rapidly anchors on the classic presentation of biliary colic: intense, self-limiting right upper quadrant/epigastric pain following a fatty meal. A bedside ultrasound confirms a gallstone, solidifying his bias. However, the supervising physician appropriately intervenes to broaden the differential, noting that inferior myocardial infarctions can present as upper abdominal pain (epigastric), which is particularly relevant in a male with a history of hypertension.
Diagnostics & Findings
- Physical Exam (Benign abdomen)
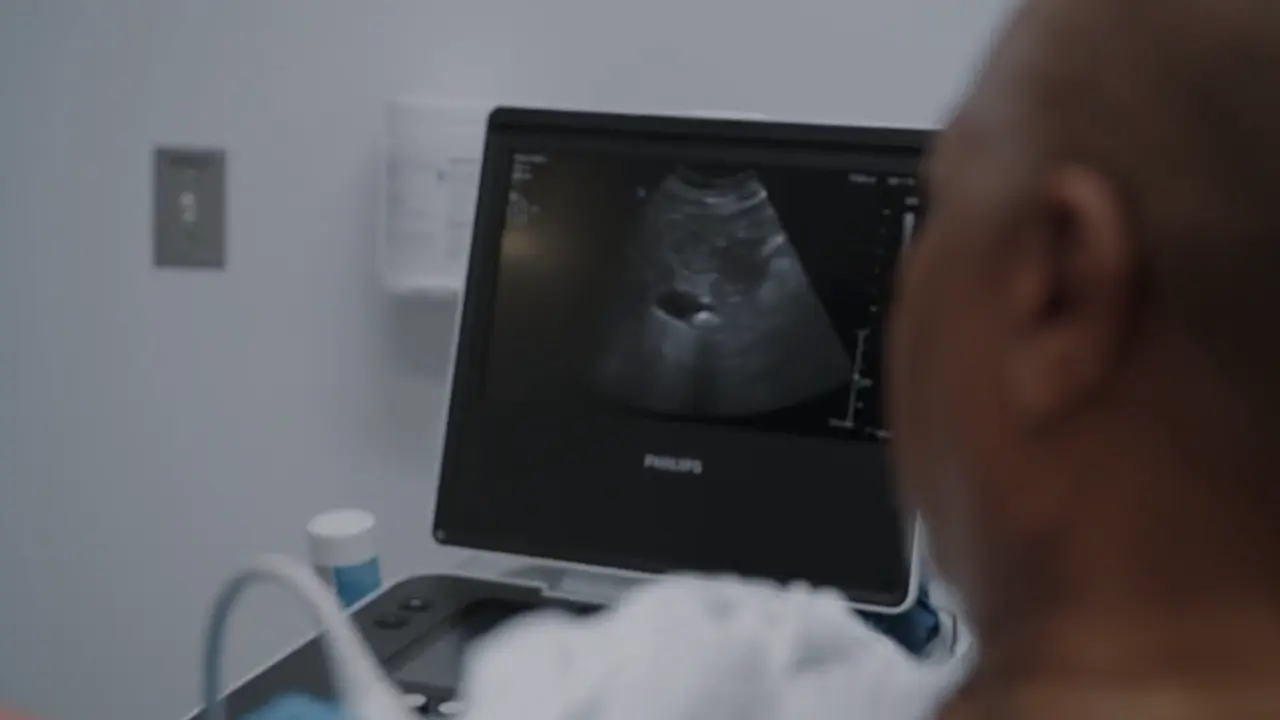
- Bedside POCUS of the Gallbladder
- Liver Function Tests (LFTs) ordered
- Pancreatic enzymes (Lipase) ordered
- 12-Lead EKG ordered
Findings:
- POCUS reveals a single gallstone in the gallbladder.
Interventions
- Patient counseled on low-fat diet to manage symptoms.
⮑ Outcome & Reassessment
Patient is currently pain-free and receptive to the dietary advice. Awaiting labs and EKG results to clear cardiac causes.
Clinical Media
Reassessment & Case Presentation
EKG results returned; medical student presents the updated case to the attending.
Reassessment & Case Presentation
EKG results returned; medical student presents the updated case to the attending.
Medical Decision Making
The EKG is clear of acute ischemic changes, lowering the suspicion for an acute myocardial infarction. The team feels reassured by the normal EKG and benign abdomen. They are now waiting purely on LFTs and Lipase to complete the GI workup before disposition.
Diagnostics & Findings
- 12-Lead EKG (Resulted)
Findings:
- EKG shows no acute ischemic changes.
Interventions
- Ice chips offered (patient declined).
⮑ Outcome & Reassessment
Patient remains comfortable and pain-free. He is eager to leave and jokingly requests alcohol.
Cardiac Arrest & Resuscitation
Patient found unresponsive in an unmonitored hallway bed with an unknown downtime.
+1
Cardiac Arrest & Resuscitation
Patient found unresponsive in an unmonitored hallway bed with an unknown downtime.
Medical Decision Making
The team discovers the patient pulseless with an unknown downtime and initiates the ACLS Cardiac Arrest algorithm for a non-shockable rhythm (Asystole). A team member asks if they should shock, which is correctly denied—you do not shock asystole. To minimize interruptions in chest compressions, they elect to drop a Laryngeal Mask Airway (LMA) rather than attempting endotracheal intubation. The team systematically works through reversible causes ('Hs and Ts'), using intra-arrest POCUS to rule out cardiac tamponade and tension pneumothorax. Hyperkalemia is considered but ruled out due to a prior normal potassium lab.
Diagnostics & Findings
- Rhythm Check (Asystole)
- Pupillary Exam (Fixed and dilated)
- Intra-arrest POCUS (Echocardiogram and Lung)
Findings:
- Monitor shows Asystole.
- Pupils are fixed and dilated, indicating prolonged brain hypoxia.
- POCUS reveals no cardiac activity, no pericardial effusion, and no signs of tension pneumothorax.
Interventions
- High-quality CPR initiated
- Laryngeal Mask Airway (LMA) inserted
- Epinephrine 1mg IV pushed x3 (every 3-5 minutes)
⮑ Outcome & Reassessment
Patient remains in asystole despite prolonged resuscitation efforts and three rounds of epinephrine. Given the unknown downtime and fixed/dilated pupils, the team prepares to terminate the code.
Clinical Media

Diagnoses & Disposition
Evolving Diagnoses
- [S01E01]Biliary Colic
- [S01E01]Rule Out Acute Coronary Syndrome (ACS)
- [S01E02]Sudden Cardiac Arrest (Asystole)
Current Disposition
Cardiac Arrest (Asystole) with unknown downtime. Resuscitation is ongoing but the team is preparing to terminate efforts (pronounce dead) following the administration of the third round of epinephrine without ROSC (Return of Spontaneous Circulation).
Casebook Analysis
Episode Context
Serves as a classic teaching moment in the ED for the fourth-year medical student, Dennis Whitaker. It demonstrates the hierarchy of medical education and the necessity of senior oversight to prevent premature closure on a diagnosis. In episode 2, the case takes a tragic turn. Milton serves as a harsh narrative lesson on the dangers of 'hallway medicine' and the unpredictability of the ED. His sudden unmonitored death underscores the reality that 'stable' patients can abruptly decompensate.
Attending's Review
Medical Accuracy
Highly accurate. Medical students frequently succumb to 'anchoring bias' when a patient presents with a textbook history (fatty meal leading to RUQ pain) and a confirmatory test (gallstone on POCUS). It is a standard-of-care ED teaching pearl to always obtain an EKG in adults, especially those with cardiovascular risk factors like hypertension, presenting with upper abdominal pain to rule out an inferior MI. The cardiac arrest sequence in S01E02 is also highly accurate to real-world ACLS protocols. The team correctly recognizes asystole as a non-shockable rhythm, prioritizes continuous compressions by choosing an LMA over intubation, administers epinephrine at the correct intervals (3-5 minutes), and uses intra-arrest POCUS to evaluate for reversible causes (the 'Hs and Ts' like tension pneumothorax or tamponade).
Complications & Errors
- Premature Closure / Anchoring Bias: MS4 Dennis Whitaker diagnosed biliary colic and was prepared to discharge the patient without considering life-threatening cardiac etiologies. The presence of a gallstone does not guarantee it is the source of the pain (asymptomatic cholelithiasis is common).
- Unmonitored Hallway Placement: Moving a 68-year-old male with cardiac risk factors and a recent presentation of upper abdominal/chest-equivalent pain into an unmonitored hallway bed is a critical system error. This led to an unwitnessed cardiac arrest with an 'unknown downtime', drastically reducing his chances of survival.
Clinical Pearls
Always obtain an EKG in older adult patients or those with cardiac risk factors presenting with upper abdominal or epigastric pain to rule out Acute Coronary Syndrome.
Beware of incidentalomas: Finding a gallstone on ultrasound is common; ensure you still rule out other critical differentials before attributing the patient's pain solely to the stone.
Biliary colic typically lasts 1-5 hours and is characterized by a steady, intense pain. If pain persists longer, suspect progression to acute cholecystitis, choledocholithiasis, or gallstone pancreatitis.
A normal EKG does not definitively rule out Acute Coronary Syndrome (ACS) or other acute cardiac events; electrical changes can be dynamic, delayed, or absent depending on the affected myocardial territory.
'Hallway medicine' introduces severe risks. Patients with potentially undifferentiated chest/abdominal pain and cardiac risk factors should remain on continuous telemetry monitoring.
During CPR, minimizing interruptions to chest compressions is paramount. Placing a supraglottic airway (like an LMA) is often preferred over endotracheal intubation if intubation would cause a prolonged pause.
In PEA/Asystole, always run through the 'Hs and Ts' using bedside ultrasound (POCUS) to rapidly identify reversible causes such as Cardiac Tamponade, Tension Pneumothorax, or severe hypovolemia.


