History of Present Illness
A 48-year-old previously healthy female presents to the ED with nausea and noticeable yellowing of her skin. The patient initially attributed the skin changes to a 100% natural sugar-beet bronzer (DHA). Triage labs revealed significantly elevated liver enzymes indicating acute hepatic inflammation. She is a strict vegan, exercises regularly, and denies all alcohol, acetaminophen, prescription medication, and illicit drug use. She denies eating raw shellfish.

Emergency Department Course
Initial Bedside Evaluation
Abnormal critical labs resulted from triage (elevated liver enzymes). Dr. Abbot assigned Dr. McKay to see the patient with intern Toomarian.
+1
Initial Bedside Evaluation
Abnormal critical labs resulted from triage (elevated liver enzymes). Dr. Abbot assigned Dr. McKay to see the patient with intern Toomarian.
Medical Decision Making
Dr. McKay attempts to systematically rule out common causes of acute hepatitis. She questions the patient on acetaminophen use (toxicology), IV drug use (Hepatitis B/C), and raw shellfish consumption (Hepatitis A). With a completely negative initial history, the etiology of the hepatic inflammation remains unknown to her.
Diagnostics & Findings
- Comprehensive Metabolic Panel (from triage)
Findings:
- Severe hepatic inflammation on labs.
- Visual jaundice (dismissed by patient as 'bronzer').
Interventions
⮑ Outcome & Reassessment
Patient is alert but nauseated. She denies all standard risk factors, complicating the diagnostic picture.
Clinical Media
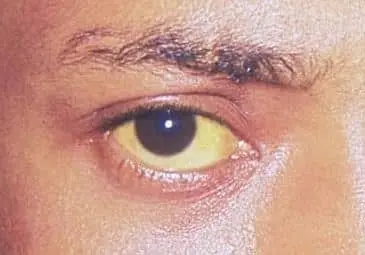
Physician Consult
Dr. McKay is stumped by the lack of risk factors and requests a second opinion.
Physician Consult
Dr. McKay is stumped by the lack of risk factors and requests a second opinion.
Medical Decision Making
McKay presents the case to second-year resident Dr. Santos and intern Dr. Whitaker, noting the patient has no risk factors for Hep A, B, C, D, or E and no alcohol/Tylenol use. Whitaker considers hypervitaminosis A from polar bear liver consumption. Knowing Santos has a knack for diagnosing 'weird stuff', McKay asks her to lay eyes on the patient. Santos agrees to a quick five-minute bedside consult.
Diagnostics & Findings
Interventions
⮑ Outcome & Reassessment
No direct patient interaction during this beat. Dr. Santos joins the diagnostic investigation.
Bedside Ultrasound & Diagnostic Breakthrough
Evaluating the physical structure of the liver to rule out chronic disease or obstruction.
+1
Bedside Ultrasound & Diagnostic Breakthrough
Evaluating the physical structure of the liver to rule out chronic disease or obstruction.
Medical Decision Making
Dr. McKay uses POCUS to assess for cirrhosis, nodules, or biliary congestion. Finding a structurally normal liver, she deduces the injury is acute and likely toxicological. Utilizing her personal diagnostic framework ('What's the stupidest thing this person could have done?'), Santos pivots to interrogating the patient's 'wellness' routine and social media health trends. She discovers she is taking massive doses of turmeric (2500mg daily). Turmeric (curcumin) is a known, though uncommon, cause of drug-induced liver injury (DILI).
Diagnostics & Findings
- Bedside Right Upper Quadrant (RUQ) Ultrasound
Findings:
- No congestion, nodules, or cirrhosis. Structurally healthy liver.
- Patient admits to taking five 500mg capsules of turmeric daily for 'detoxing'.
Interventions
- Advise patient to immediately cease taking turmeric.
⮑ Outcome & Reassessment
Patient is shocked that a natural spice could cause organ failure.
Clinical Media
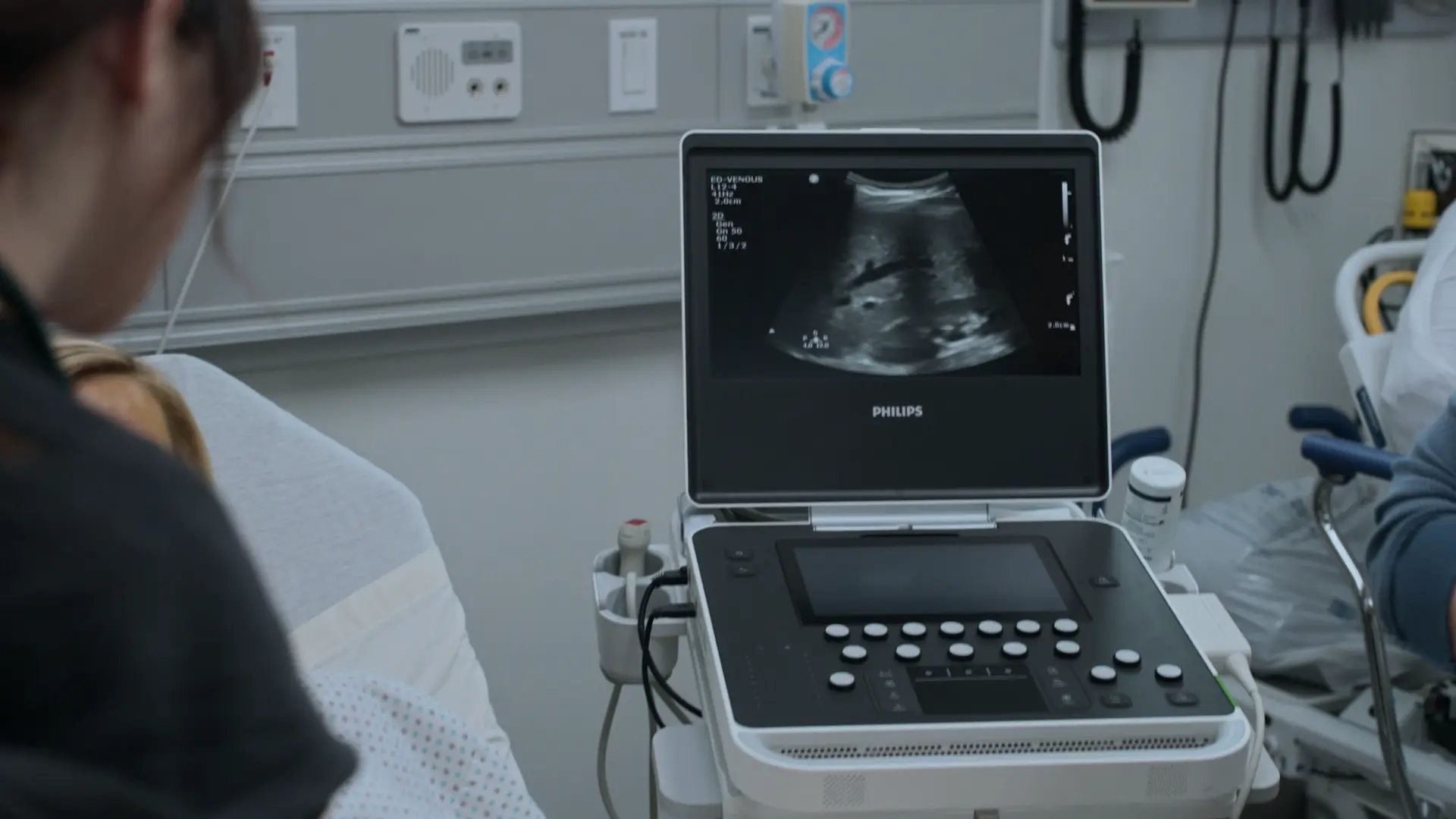
Lab Review & Disposition
Coagulation panel results return from the lab.
Lab Review & Disposition
Coagulation panel results return from the lab.
Medical Decision Making
Dr. McKay reports back to Toomarian. The elevated INR (2.2) indicates that the liver's synthetic function is becoming compromised, pushing the diagnosis toward severe acute liver injury or impending acute liver failure. McKay formulates the disposition: the patient requires skip the turmeric, and inpatient admission for close monitoring of LFTs and coag panel.
Diagnostics & Findings
- Coagulation Panel (PT/INR)
Findings:
- INR is elevated at 2.2
Interventions
- Admit to inpatient Med-Surg or Step-Down for monitoring.
- Strict discontinuation of all turmeric and supplements.
⮑ Outcome & Reassessment
McKay hands off the case to Toomarian to admit the patient.
Diagnoses & Disposition
Evolving Diagnoses
- [Initial Bedside Evaluation]Acute Hepatitis of Unknown Etiology
- [Bedside Ultrasound & Diagnostic Breakthrough]Drug-Induced Liver Injury (DILI) secondary to Turmeric Megadosing
Current Disposition
Admitted to the hospital for monitoring of LFTs and Coagulation panel due to elevated INR (2.2) and risk of acute liver failure.
Casebook Analysis
Episode Context
Mrs. Davis serves as a diagnostic 'mystery of the week' B-plot. The case highlights Dr. Santos's cynical but highly effective diagnostic framework ('What's the stupidest thing this person could have done?'), showcasing her ability to uncover hidden toxidromes that strictly algorithmic doctors (like Dr. McKay in this instance) might miss. It also provides a sharp critique of unregulated wellness culture.
Attending's Review
Medical Accuracy
Highly accurate. Turmeric (and its active compound curcumin) has been increasingly recognized in recent medical literature as a potential cause of Drug-Induced Liver Injury (DILI). This is especially true when taken in high supplement doses or combined with black pepper extract (piperine) which massively increases absorption. Furthermore, the progression to check an INR to assess hepatic synthetic function is exactly the standard of care for evaluating acute liver injury.
Complications & Errors
- The patient fell victim to unregulated 'wellness' trends, assuming 'natural' equated to 'safe', resulting in severe iatrogenic/supplement-induced organ damage.
Clinical Pearls
When evaluating liver injury, it is crucial to distinguish between a cytolytic syndrome (hepatocellular injury) and cholestasis. Cytolysis involves direct hepatocyte destruction marked by severely elevated AST and ALT along with a mixed hyperbilirubinemia (both indirect/unconjugated and direct/conjugated bilirubin are elevated). Conversely, cholestasis involves impaired bile flow marked by elevated Alkaline Phosphatase (ALP) and a predominantly direct (conjugated) hyperbilirubinemia. Turmeric toxicity can present with either pattern or a mixed picture; distinguishing between them helps narrow down potential toxicological differentials and guides management.
Always ask patients explicitly about 'supplements, vitamins, and herbal remedies'. Many patients do not consider these to be 'medications' and will answer 'no' when asked if they take any prescription drugs.
Turmeric/Curcumin is a well-documented cause of idiosyncratic drug-induced liver injury (DILI). Suspect it in health-conscious patients presenting with unexplained acute hepatitis.
In the setting of acute hepatitis, transaminases (AST/ALT) indicate inflammation, but PT/INR indicates synthetic function. An elevated INR (like 2.2) is a massive red flag for impending acute liver failure and necessitates admission.